30%的女性一生中会遭遇异常子宫出血(AUB),而子宫腺肌病与子宫肌瘤是导致AUB的两大最常见良性病因。这两种疾病症状相似,但治疗方案选择直接影响生育保留、症状控制效果——如何精准鉴别?药物治疗该选连续还是间歇方案?

图源:《Scientific Reports》
埃及阿西尤特大学团队2025年发表于《Scientific Reports》的前瞻性研究(NCT05153928),用100例临床数据给出了明确答案:宫腔镜是鉴别诊断的“利器”,炔诺酮连续给药控制月经过多更优!本文提炼核心证据,直接落地临床实操。
研究核心信息速览
01研究对象
100例绝经前AUB女性,平均年龄41.3岁,85%合并月经过多,50%有痛经,34%存在性交痛,18%伴排便痛(基线VAS评分见下图)。
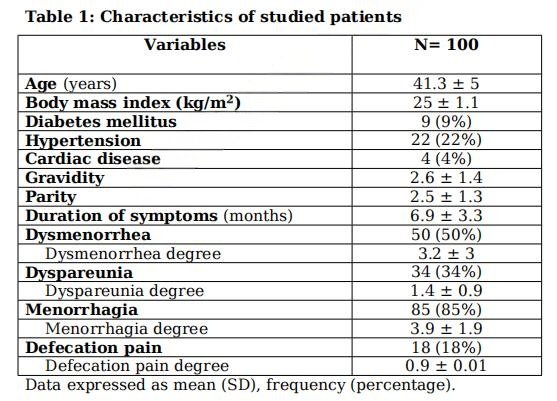
图源:《Scientific Reports》
关键纳入标准:25-45岁、超声提示子宫腺肌病/黏膜下肌瘤、月经规律;排除妊娠/哺乳、卵巢肿瘤、盆腔炎及内分泌疾病。
02研究设计
诊断方法:所有患者均行宫腔镜检查,以病理结果为金标准,评估宫腔镜鉴别腺肌病与肌瘤的准确性;
治疗方案:
◆连续组(46例):炔诺酮第5-21天连续给药;
◆间歇组(54例):炔诺酮第16天起连续给药10天;
随访指标:治疗3个月后,通过VAS评分评估痛经、性交痛、月经过多、排便痛改善情况。
核心结果:诊断+治疗双突破
01宫腔镜:鉴别腺肌病/肌瘤的“精准工具”
以病理诊断为基准,宫腔镜的诊断效能堪称优异,尤其特异性超95%,大幅降低误诊率:
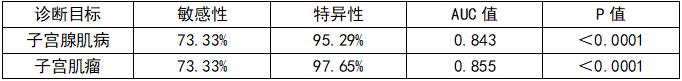
临床意义:当超声提示“子宫占位+AUB”但无法明确是腺肌病还是肌瘤时,宫腔镜可直接可视化宫腔内病变,明确病灶数量、大小、位置,为手术(如肌瘤切除术)或药物选择提供精准依据。
02炔诺酮治疗:连续方案控制月经过多更高效
两种方案均能改善症状,但在核心痛点“月经过多”上,连续给药优势显著:
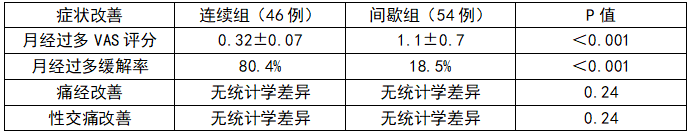
关键证据:ROC曲线分析显示,炔诺酮预测月经过多缓解的AUC达0.793(敏感性80.43%,特异性81.48%),是控制AUB的可靠药物选择。
03额外发现:腺肌病患者症状更顽固
➱病理确诊的15例腺肌病患者,相比85例肌瘤患者:
◆症状持续时间更长(8.6个月vs6.6个月,P=0.04);
◆基线痛经、性交痛、排便痛评分更高(均P<0.001);
◆治疗后症状改善幅度仍低于肌瘤组,但两种给药方案对腺肌病的疗效无差异。
临床启示:直接落地的3条实操建议
01诊断流程优化
超声初筛:发现子宫占位+AUB,先评估病灶位置(黏膜下肌瘤优先考虑宫腔镜);
宫腔镜确诊:超声结果不确定、需保留生育功能、计划药物治疗前,优先行宫腔镜检查,明确病变类型;
联合诊断:绝经前后AUB可联合经阴道超声+宫腔镜,诊断一致性Kappa值达0.784(单独超声Kappa=0.475,单独宫腔镜Kappa=0.669)。
02炔诺酮方案选择
优先选连续方案(第5-21天):需快速控制月经过多、严重影响生活质量时;
选间歇方案(第16-25天):希望维持规律月经、症状较轻的年轻患者;
注意事项:炔诺酮价格低廉、副作用温和,适合不愿手术或需术前预处理的患者。
03特殊人群管理
腺肌病患者:症状持续久、疼痛更重,建议延长随访时间,必要时联合其他治疗(如GnRH-a);
肌瘤患者:黏膜下肌瘤合并月经过多,宫腔镜术后可辅助炔诺酮预防复发。
研究局限性与未来方向
局限:单中心研究、样本量100例、随访仅3个月,长期疗效和安全性需进一步验证;
建议:未来需开展多中心大样本研究,探索宫腔镜在不孕患者中的应用价值,以及炔诺酮长期使用的依从性和副作用。
总结
宫腔镜是鉴别子宫腺肌病与子宫肌瘤的高效工具(特异性超95%),炔诺酮连续给药方案控制AUB核心症状“月经过多”更优——这组证据为临床提供了“诊断+治疗”的一体化解决方案,尤其适合基层医院和门诊快速决策。
对于AUB患者,记住核心逻辑:超声不确定就选宫腔镜,月经过多就用连续炔诺酮,既保证精准性,又兼顾疗效和经济性。
参考文献:
Lebduska, E., D. Beshear, and B.M. Spataro. Abnormal uterine bleeding. Medical Clinics, 2023, 107(2): p. 235-246.
Singh, S., P. Kumar, S.S. Rathore, Y. Singh, and N. Garg. Contemporary approaches in the management of uterine leiomyomas. European Journal of Obstetrics & Gynecology and Reproductive Biology, 2023, 287: p. 195-210.
Bourdon, M., P. Santulli, L. Marcellin, C. Maignien, L. Maitrot-Mantelet, C. Bordonne, et al. Adenomyosis: an update regarding its diagnosis and clinical features. Journal of gynecology obstetrics and human reproduction, 2021, 50(10): p. 102228.
Di Spiezio Sardo, A., G. Calagna, F. Santangelo, B. Zizolfi, V. Tanos, A. Perino, et al. The role of hysteroscopy in the diagnosis and treatment of adenomyosis. BioMed research international, 2017, 2017(1): p. 2518396.
Gordts, S., G. Grimbizis, and R. Campo. Symptoms and classification of uterine adenomyosis, including the place of hysteroscopy in diagnosis. Fertility and sterility, 2018, 109(3): p. 380-388. e1.
Gulisano, M., F.A. Gulino, G.G. Incognito, M. Cimino, V. Dilisi, A. Di Stefano, et al. Role of hysteroscopy on infertility: The eternal dilemma. Clinical and Experimental Obstetrics & Gynecology, 2023, 50(5): p. 99.
Boruah, A.M., D. Banerjee, F. Bhardwaj, S. Mallya, R. Singal, S. Sharma, et al. Effect of norethindrone dose and duration in the management of abnormal uterine bleeding: a narrative review and case report. Drugs in Context, 2024, 13.
Ignaszak-Kaus, N., K. Chmaj-Wierzchowska, A. Nowak, K. Wszołek, and M. Wilczak. An Overview of Outpatient Hysteroscopy. Clinical and Experimental Obstetrics & Gynecology, 2022, 49(8): p. 181.
De Silva, P., L. Wilson, A. Carnegy, P. Smith, and T. Clark. Cervical dilatation and preparation prior to outpatient hysteroscopy: a systematic review and meta‐analysis. BJOG: An International Journal of Obstetrics & Gynaecology, 2021, 128(7): p. 1112-1123.
Hou, J.-H., B.-J. Lu, Y.-L. Huang, C.-H. Chen, and C.-H. Chen. Outpatient hysteroscopy impact on subsequent assisted reproductive technology: a systematic review and meta-analysis in patients with normal transvaginal sonography or hysterosalpingography images. Reproductive Biology and Endocrinology, 2024, 22(1): p. 18.
Wang, Y., Z. Tang, C. Wang, X. Teng, and J. He. Whether hysteroscopy improves fertility outcomes in infertile women: a meta-analysis and systematic review. Frontiers in endocrinology, 2024, 15: p. 1489783.
Foreste, V., A. Gallo, A. Manzi, C. Riccardi, J. Carugno, and A.D.S. Sardo. Hysteroscopy and retained products of conception: an update. Gynecology and minimally invasive therapy, 2021, 10(4): p. 203-209.
Ding, Y., Y. Han, S. Zhang, and X. Shi. The incidence of unexpected uterine malignancies in hysterectomies carried out for benign indications. Journal of Cancer Research and Clinical Oncology, 2023, 149(8): p. 4339-4345.
Nicula, R., D. Diculescu, C.C. Lencu, R. Ciortea, C.E. Bucuri, I.A. Oltean, et al. Accuracy of transvaginal ultrasonography compared to endometrial biopsy for the etiological diagnosis of abnormal perimenopausal bleeding. Clujul Medical, 2017, 90(1): p. 33.
Al Nemer, A.M., M.I. Al Bayat, and N.H. Al Qahtani. The accuracy of endometrial sampling for the diagnosis of patterns of endometrial pathology in women presenting with abnormal uterine bleeding: More conservative therapeutic approaches. Saudi medical journal, 2019, 40(8): p. 815.
De Franciscis, P., G. Riemma, A. Schiattarella, L. Cobellis, M. Guadagno, S.G. Vitale, et al. Concordance between the hysteroscopic diagnosis of endometrial hyperplasia and histopathological examination. Diagnostics, 2019, 9(4): p. 142.
Tuersun, B. and Q. Zhang. Application of vaginal ultrasound and hysteroscopy in the diagnosis of perimenopausal endometrial lesions. Clinical and Experimental Obstetrics & Gynecology, 2024, 51(6): p. 128.
Wang, Y. and Q. Long. Diagnostic Value of Vaginal Ultrasound under Improved Clustering Algorithm combined with hysteroscopy in abnormal uterine bleeding. Computational Intelligence and Neuroscience, 2022, 2022(1): p. 6951692.
Bettocchi, S., L. Nappi, O. Ceci, A. Santoro, N. Fattizzi, C. Nardelli, et al. The role of office hysteroscopy in menopause. The Journal of the American Association of Gynecologic Laparoscopists, 2004, 11(1): p. 103-106.
责编:霍盼


















