An impacted fetal head (IFH) is an unpredictable obstetric emergency during cesarean delivery, associated with significant risks of maternal and neonatal complications.
This article provides clear, practical management strategies based on the latest evidence-based medicine, particularly the most recent literature from the Royal College of Obstetricians and Gynaecologists (RCOG) in 2025 and the content related to IFH during cesarean delivery in UpToDate.
PART 01 Definition, Epidemiology, and Risk Factors
1. Definition
There is currently no internationally unified definition for IFH. Based on clinical practice, a practical definition is: IFH can be diagnosed when the obstetrician is unable to deliver the fetal head using conventional delivery techniques and requires additional maneuvers and/or uterine relaxation to disimpact the head.
2. Epidemiology
The incidence of IFH is on the rise. The latest UK research data indicates that IFH may be implicated in up to 10% of unplanned cesarean deliveries (1.5% of all births) and 16% to 32% of cesarean deliveries performed in the second stage of labor.
3. Risk Factors
❖ Primary Factors: Cesarean delivery performed at full cervical dilation (second stage of labor), cesarean delivery following failed instrumental delivery (forceps or vacuum).
❖ Associated Factors: Prolonged labor, use of oxytocin, abnormal fetal head position, presence of caput succedaneum or significant fetal head molding.
❖ Important Note: IFH is not exclusive to the second stage; over 50% of IFH-related complications occur during cesarean deliveries in the first stage of labor, and there are even rare reports in pre-labor cesarean sections.
PART 02 Maternal and Neonatal Complications
Improper management of IFH can lead to severe outcomes and is a significant cause of obstetric litigation.
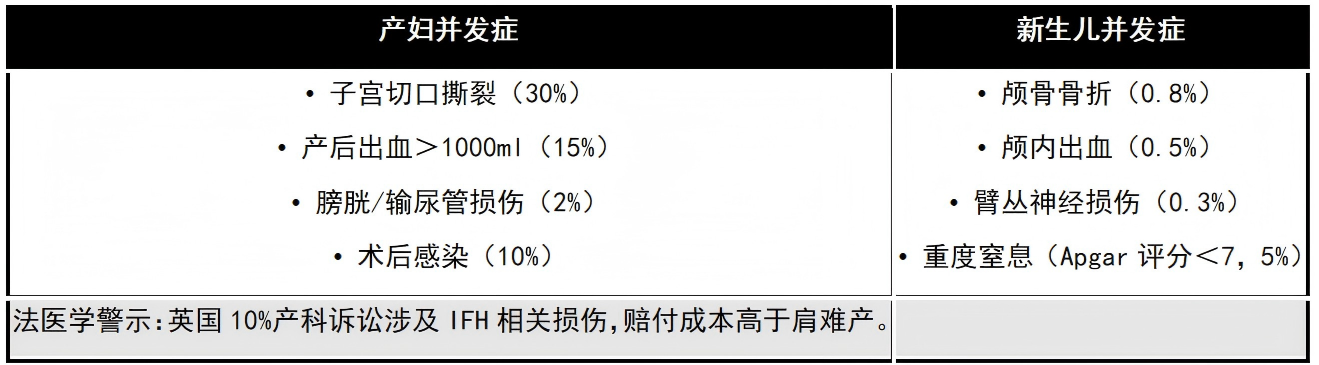
❖ Maternal Complications: Uterine incision extension, severe obstetric hemorrhage (requiring transfusion), bladder and ureter injuries, postpartum infection, broad ligament hematoma. Long-term, it may increase the risk of spontaneous preterm birth in future pregnancies.
❖ Neonatal Complications: Skull fracture, subgaleal hematoma, intracranial and retro-orbital hemorrhage, brachial plexus injury, spinal cord injury. Delayed delivery can lead to hypoxic-ischemic encephalopathy, and in severe cases, perinatal death.

PART 03 Preventive Measures and Preoperative Preparation
The core of prevention lies in anticipation and preparation in high-risk situations.
1. Multidisciplinary Team Communication:
◆ Once a decision is made to perform a cesarean section on a patient suspected to be at high risk for IFH, the delivery plan should be explicitly discussed during the preoperative briefing.
◆ Ensure the presence of anesthesia, nursing, obstetric, and neonatal personnel.
2. Patient Positioning and Operating Table Optimization:
◆ Place the patient in a head-down, feet-up supine position (Trendelenburg).
◆ Appropriately lower the operating table height and provide a footstep for the surgeon to optimize mechanical force transmission.
◆ If a combined abdominal-vaginal delivery is planned, position the patient in the frog-leg position while maintaining a sterile field.
3. Application of Preventive Devices (Current Evidence Status):
❖ Fetal Pillow: An inflatable balloon device designed to be inserted vaginally beneath the fetal head and inflated before cesarean section to elevate the head.
❖ Evidence Evaluation: A 2025 BJOG systematic review noted that the certainty of evidence from studies comparing the fetal pillow with no preventive measures is low to very low. Existing studies have a high risk of bias and heterogeneity, and some key studies have been retracted. Meta-analysis showed that the fetal pillow did not significantly reduce the incidence of uterine incision extension, postpartum hemorrhage, or neonatal birth trauma.
❖ Clinical Recommendation: Based on current evidence, the fetal pillow should not be promoted for routine clinical practice outside of clinical trials. The UK National Institute for Health and Care Excellence (NICE) recommends its use only under special arrangements for clinical monitoring or research.
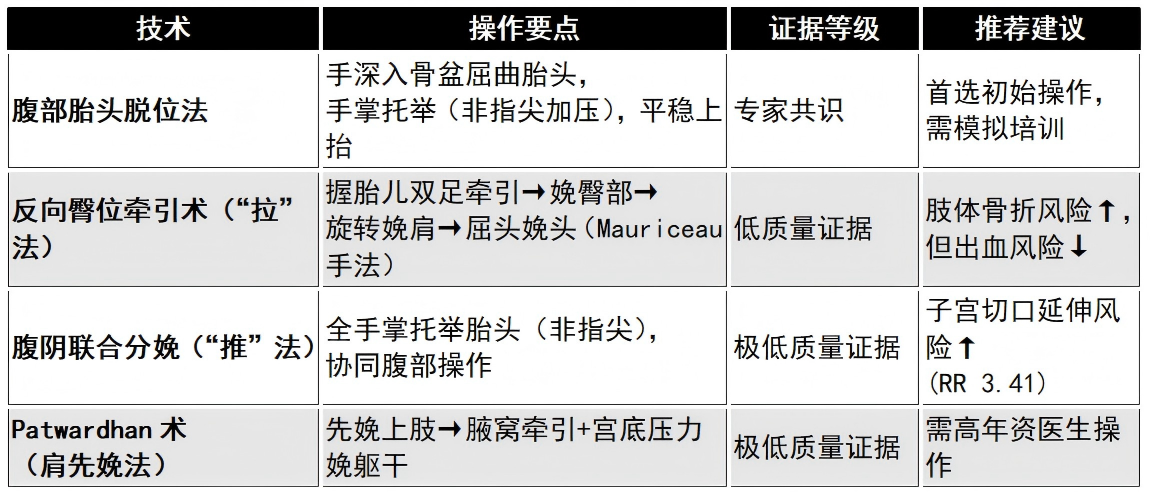
PART 04 Tiered Management Techniques
Once IFH is diagnosed after hysterotomy, a systematic, stepwise management principle should be followed. The following maneuvers should be mastered through simulation training.
Step 1: Initial Assessment and Basic Maneuvers (Abdominal Head Disimpaction)
Before attempting any maneuvers, consider using a short-acting tocolytic (e.g., sublingual nitroglycerin) if uterine contractions are strong, to create space for manipulation.
➱ Abdominal Head Disimpaction: This is the primary and foundational technique. The key is to utilize the fact that the pelvic transverse diameter is greater than the anterior-posterior diameter.
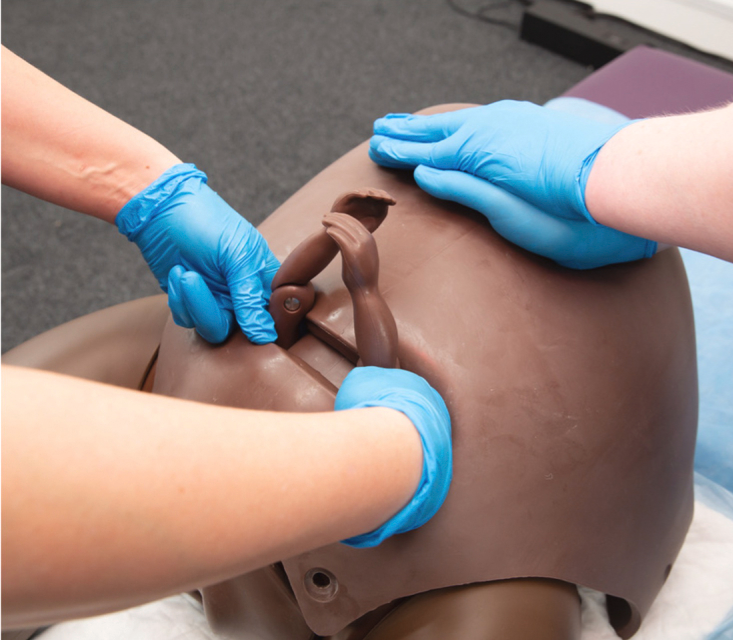
❖ Key Points: The surgeon's hand enters from the side of the fetal head, placing the palm against the fetal face or occiput to flex the head. Then, keeping the arm straight and parallel to the maternal torso, apply steady force toward the maternal head (not vertically upward) to lift the head out of the pelvis and guide it toward the uterine incision.
❖ Avoid: Avoid using the wrist against the lower uterine segment as a fulcrum, as this can easily cause cervical tears.
Step 2: Escalation Maneuvers (When Basic Maneuvers Fail)
Although the certainty of evidence from comparative studies is generally low to very low, existing data tend to suggest that "pull" techniques may be associated with a lower risk of some maternal complications compared to "push" techniques.
➱ Reverse Breech Extraction ("Pull" Technique)
❖ Procedure: The surgeon inserts a hand into the uterine fundus, grasps one or both fetal feet, and applies traction along the axis of the fetal legs to deliver the fetal body as a breech, followed by the head.
❖ Evidence: Meta-analysis suggests this technique may significantly reduce the risk of uterine incision extension (RR 3.41), postpartum hemorrhage (RR 2.21), and transfusion (RR 2.75) compared to the push technique.
❖ Note: Requires formal training to avoid inappropriate traction leading to fetal femur or tibia/fibula fractures.
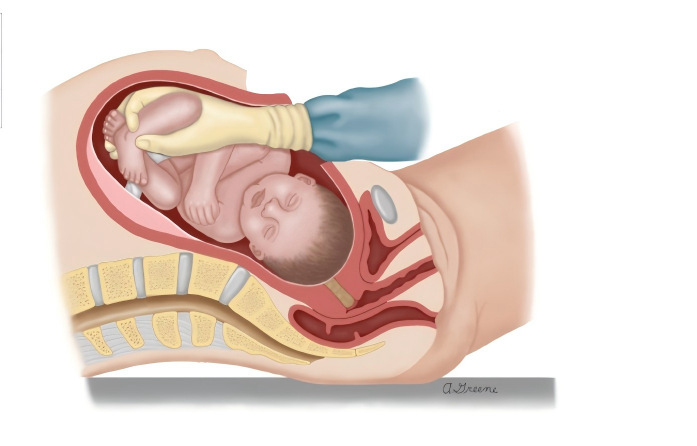
图片来源:uptodate
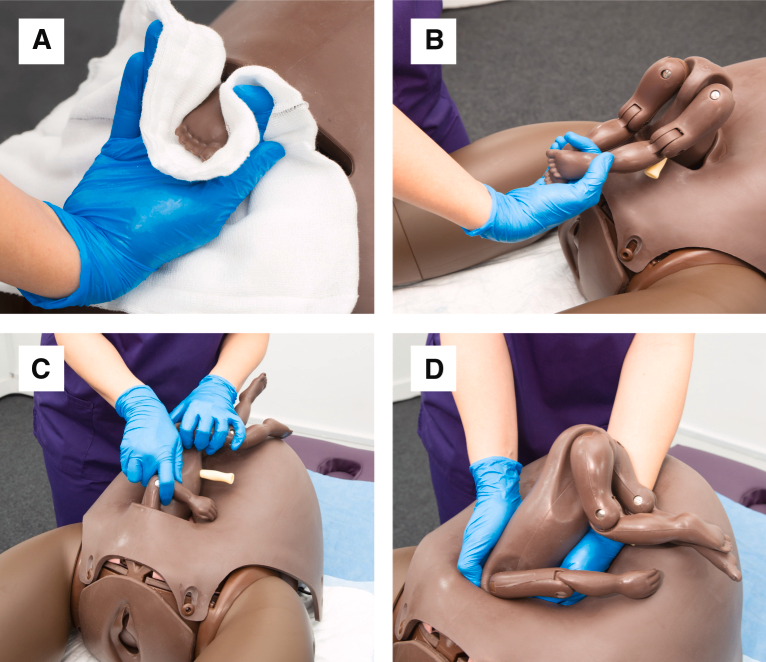
图片来源:AJOG
➱ Combined Abdomino-Vaginal Delivery ("Push" Technique)
❖ Procedure: An assistant, wearing sterile gloves, inserts the entire hand in a cupped shape into the vagina to support and push the fetal head upward, while the surgeon assists from the abdomen.
❖ Crucial: The palm must be used to apply force evenly. Absolutely avoid using one or two fingers to apply localized pressure, to prevent point pressure on the fetal skull leading to fracture.
❖ Risk: This technique is associated with an increased risk of uterine incision extension. Data from randomized trials indicate relatively higher risks of maternal infection, hemorrhage, and other complications.
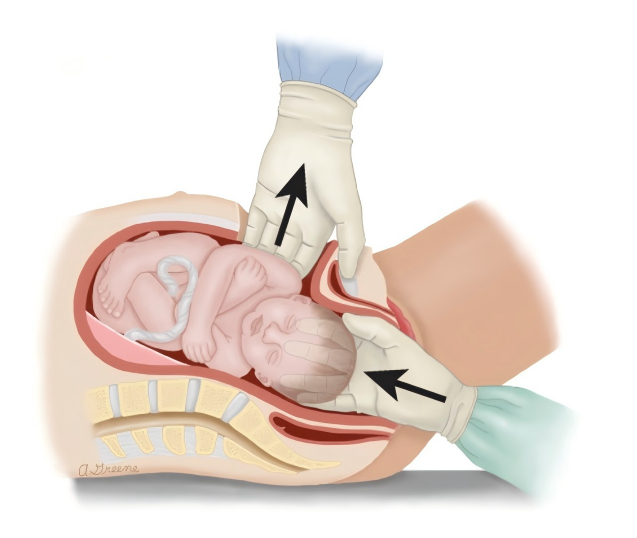
图片来源:uptodate
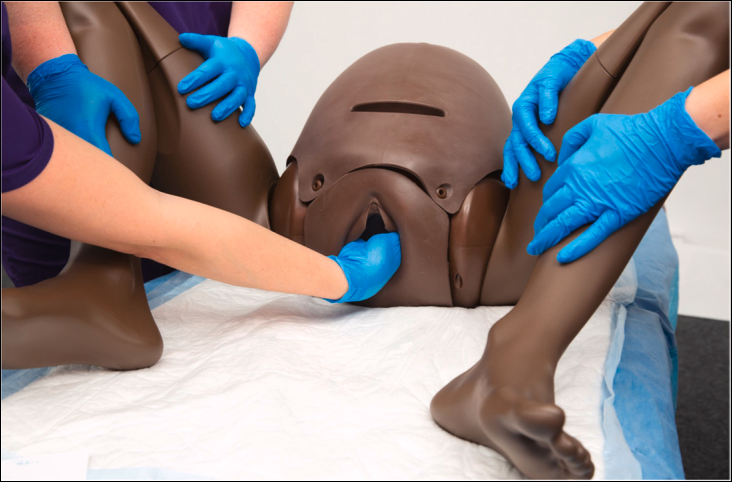 \
\
图片来源:AJOG
➱ Patwardhan Technique (Shoulder First Delivery)
❖ This is a modification of reverse breech extraction, delivering the fetal arms first, followed by the trunk. It is more commonly used in India but lacks extensive validation and training support in other regions.
图片来源:AJOG
➱ Uterine Incision Extension (T or J-shaped Incision)
❖ If none of the above maneuvers succeed in delivering the fetus within 5 minutes of hysterotomy, or if there is an uncontrollable tendency for incision tearing, decisively perform a uterine incision extension.
PART 05 Not Recommended Techniques
Based on existing evidence and expert consensus, the following techniques carry clear risks and should be avoided:
☒ Vacuum Extraction: Difficult to place safely during cesarean section, and there are reports of potential severe fetal injuries such as intracranial hemorrhage.
☒ Single Blade Forceps Assistance: No evidence supports its safety and efficacy.
☒ Bladder Filling: No evidence supports its use.
PART 06 Non-Technical Skills and System Support
Communication and Teamwork:
☑ Clear Declaration: The lead surgeon should calmly declare "Impacted Fetal Head," initiating the team's emergency response.
☑ Closed-Loop Communication: Use closed-loop communication when assigning roles and executing tasks to ensure instructions are accurately understood and carried out.
☑ Structured Documentation: Postoperatively, the techniques used, sequence of maneuvers, time taken, and outcomes should be documented in detail. Using a structured form is recommended to facilitate clinical debriefing, quality improvement, and addressing medico-legal issues.
☑ Simulation Training: Given the unpredictability of IFH, high-fidelity, multidisciplinary simulation training is key to enhancing team preparedness and confidence. Training should cover all tiered management techniques and teamwork processes.
Summary and Outlook
Managing IFH during cesarean delivery relies on adequate preoperative anticipation, a systematic tiered management plan, proficient operative techniques, and efficient multidisciplinary teamwork. Frontline obstetricians should recognize the limitations of most current evidence and integrate patient-specific circumstances with their own technical expertise in clinical decision-making. There is an urgent need for well-designed, large-scale randomized controlled trials based on a unified definition to clarify the efficacy and safety of various interventions.
References:
1.Management of the Impacted Fetal Head at Caesarean Birth (2nd edition, 2025).BJOG 2025.
2.uptodate:剖宫产中胎头深嵌与高浮的处理。
(图片来源:uptodate:剖宫产中胎头深嵌与高浮的处理。)
About the Translator

Editor: Lily














